Millions of women pay the price for their killer heels in the form of bunions, a complaint affecting one in three of us.
The condition, which is thought to run in families and affects men, too, causes the big toe bone to swing sideways at an angle towards the second toe.
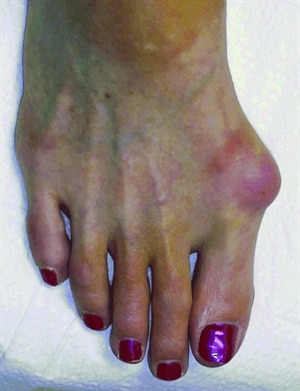
The long foot bone beneath it (called a metatarsal) is driven outwards, forming a sore and unsightly lump on the side of the foot.
In some cases, the surgeon also has to fuse the joint, drastically reducing flexibility.
The latest treatment is with specially designed surgical screws that are buried in the bone and do not need to be removed, meaning a lower risk of infection and a more comfortable recovery.
In another operation, the surgeon cuts a wedge from the inside of the long foot bone that’s swinging out, so it sits straight again.
The removed wedge of bone is attached to the outside of the bone and acts like a buttress, reinforcing and preventing it from moving out again.
Again this means no wire, and also avoids fusing the joint.
‘This offers an excellent alternative for younger patients with bad bunions as it keeps all the foot joints intact,’ says podiatric surgeon Ralph Graham.
BIG TOE ARTHRITIS
In arthritis of the big toe, wear and tear to the joint causes it to become inflamed, and tiny sections of bone — called bone spurs — grow on the top of the joint.
The body grows these in an attempt to repair a damaged joint, but it does more harm than good.
The spurs collide and pinch the joint when you walk, bend the toe and rub on footwear.
Surgeons have been working to develop a way to treat this without open surgery and avoiding fusing the bone, which leaves the toe rigid.
They have started operating through a tiny, 6mm incision with a special drill that reduces the spur to a paste, and they then massage this out.
‘Patients can put weight on the foot immediately and wear normal shoes within three to four days instead of needing surgical shoes for weeks,’ says David Redfern, orthopaedic surgeon.
‘Around 80 per cent of patients say they are happy or very happy with the results.’
BUNIONETTES
They are less well known than bunions, but surprisingly one in five of us develops bunionettes —bumps on the outside of the foot where the little toe meets the long toe bones of the foot.
The condition was once called tailor’s bunions — as they worked cross-legged, the outside edge of their feet pressed into the ground, causing a pressure point.
Like bunions, bunionettes are genetic, but can be made worse by tight high heels.
Keyhole techniques for bunionettes have been available for just a few years.
Here, the surgeon makes a 3mm to 4mm incision on top of the foot and drills away the bump with a fine drill burr, squeezing the shavings out through the incision.
As the incision is so tiny, patients need only a small plaster.
‘This has transformed practice,’ says David Redfern.
‘Patients can wear normal footwear within a few days and go back to work immediately.’
MORTON’S NEUROMA
This excruciating condition occurs when a nerve gets trapped between the bones of the foot, resulting in pain on the ball of the foot and at the base of the toes.
High heels and hormonal changes, such as the menopause, can exacerbate the problem.
Treatments include supports worn inside the shoe and injections of steroid, alcohol and liquid nitrogen into the nerve.
But if these don’t work, it’s possible to have a 15-minute operation, where surgeons remove a fingernail-sized portion of the nerve.
Studies show it’s effective in 80 per cent of cases.
‘Patients who have suffered years of excruciating pain can find the problem has gone for good,’ says Mike O’Neill, podiatrist and spokesman for the College of Podiatry.
‘But in 20 per cent of cases, the nerve stump can regrow, so it has to be done again.’
There’s also cryosurgery, where the surgeon treats the thickened nerve using a freezing probe cooled to minus 70c under a local anaesthetic.
FLAT FEET
Around one in five adults has flat feet, when the major tendon under the foot has failed — often through wear and tear as we age, or injury.
The heel and toes start to slide outwards, and the abnormal position means bones start to rub against each other, which can cause arthritis and pain.
A newer technique developed in the U.S. around two years ago, and available just at one centre, the BMI Sefton in Liverpool, means surgeons can remove the damaged tendon and replace it with a tendon taken from the smaller toes.
This is wrapped round the bone in the arch of the foot to restore the foot’s natural arch.
This is a great improvement on other methods, in which four small bones are fused, meaning patients can no longer rotate their foot.
Surgeons can also use a hamstring tendon from the back of the leg to replace a ligament on the inside of the foot, which restore the natural arch.
HAMMER TOES
Around one million Aussies have hammer toes, where the smaller toes of the foot become bent over like the head of a hammer.
The condition can run in families, and can be made worse by tight footwear and conditions such as rheumatoid arthritis.
It can cause the top of the toe to rub painfully against the top of the shoe, or results in the patient walking with their weight on the balls of the feet, causing discomfort.
Traditional surgery involves removing the ‘knuckle’ or middle joint of the toe, then holding the toe straight with a thick wire for six weeks while the two bone ends grow together and heal.
The wire sticks out of the toe, meaning the patient must wear an open-toed surgical sandal.
There is also a 5 per cent risk that the wire can change position or even come out, meaning the operation must be redone.
The new Smart Toe implant is a 1cm metal clip that is inserted into the toe.
Its ‘smart metal’ expands at body temperature, gripping the two bone ends together so they heal straight.
‘Patients can bathe the foot and wear normal footwear after just two weeks,’ says Nick Cullen, consultant orthopaedic foot and ankle surgeon.
‘And because there are no wires, the patient does not have to come back to have them removed, and the risk of infection is far lower — less than 1 per cent.’
by Susan Floyd


